Andrology

Articles published by Dr. Alexandre Miranda in the official journal of the American Society of Andrology on male hormone replacement
Men's Health
Men live 7.59 years less than women. Data from the Brazilian Institute of Geography and Statistics (IBGE) reveals that although life expectancy for men increased from 63.15 to 69.42 years from 1991 to 2009, it is still well below the average for women.
The main cause of death in men was ischemic heart disease, including acute myocardial infarction. In all, 49,128 men died from this cause. Cerebrovascular diseases were the second leading cause of death for men, with 45,180 deaths. The two causes can be grouped together as cardiovascular diseases, totaling 94,308 deaths in men. These diseases are mainly caused by endothelial lesions (blood vessels).
These lesions are first visible in the smaller vessels, such as the penile artery (1-2 mm). Occlusion of these vessels causes erectile sexual dysfunction (ESD) or lack of erection.
Ponholzer et al showed that coronary artery disease is 65% higher in men with moderate to severe SD than in normal men.
Inman et al observed that patients with SDB have an 80% higher risk of acute myocardial infarction compared to normal individuals. Men between the ages of 40 and 49 with moderate to severe ESRD have a 50 times greater risk of developing cardiovascular disease.
In addition to ESRD, we have another important factor for cardiovascular disease in men: the reduction in testosterone with age, known as Late Onset Hypogonadism (LOH), which affects 6% of the male population at the age of 40 and 12.3% at the age of 69.
Recent data in the literature shows that the age-related increase in the risk of coronary heart disease appears in conjunction with a reduction in testosterone.
Patients undergoing hormone blockade, i.e. removal of testosterone from circulation (castration) due to prostate cancer, are at high risk of coronary heart disease due to the marked reduction in serum testosterone. Male hormone replacement is an important factor in the quest to reduce the incidence of cardiovascular disease. It leads to a reduction in cholesterol, greater exercise tolerance, greater sensitivity to insulin action (helping to control diabetes), a reduction in the thickness of the artery wall and a reduction in inflammatory factors in the endothelium (vessel).
Considering the above, every man must recognize that he is neither immortal nor immune to disease. Recognizing your limitations and seeking appropriate medical care is essential to living a healthy life.
MEN'S SEXUAL HEALTH
Bate Papo na Saúde program, Canal Saúde - Fiocruz
Aired on 30/03/2015
Male Hormone Replacement
Hormone replacement will be necessary in patients with hypogonadism. This is characterized by a clinical condition in which low testosterone levels are found in association with specific signs and symptoms. When hypogonadism occurs in older men, the condition is generally called andropause or late onset hypogonadism, also referred to as LOH (Late Onset Hypogonadism). It is estimated that hypogonadism affects 6% of the male population by the age of 40 and 12.3% by the age of 69.
In the United States alone, approximately 2.4 million people are affected.
The diagnosis is made when there are low levels of testosterone in the blood with associated signs and symptoms:
- Fatigue/weakness.
- Reduced libido.
- Reduction of "energy".
- Erectile dysfunction (erection problems).
- Reduced muscle mass.
- Osteoporosis.
- Increased abdominal fat.
- Cognitive impairment (forgetfulness, slow thinking).
- Insomnia
Hormone replacement improves and reverses all the associated symptoms. However, it must be accompanied by regular visits to your urologist. Some changes can arise with the continued use of testosterone and need to be monitored continuously.
Watch Dr. Alexandre Miranda's interview on testosterone deficiency in aging men, shown on the program Ligado em Saúde - Canal Saúde, Fiocruz.
Erectile Dysfunction
The prevalence in the male population is 16%, between 20 - 75 years of age; 15%, between 40 - 49 years of age and 30%, between 60-69 years of age. Its incidence becomes more significant after the age of 50 [1]. The psychological impact of erectile dysfunction is immense, as are problems in marital relationships.
There are many causes, involving vascular factors (blood vessels), neurological factors, psychological factors, associated diseases (e.g. diabetes) and many others.
There are various treatments available, but only after careful medical assessment can we identify the causes and plan your personalized treatment.
%
of men are affected
Also watch Dr. Alexandre Miranda talking about erectile dysfunction
Penile Prosthesis
Penile prostheses are devices implanted inside the penis of men with erectile dysfunction, allowing them to achieve erections. These implants are generally recommended when less invasive treatments have failed. There are two types of penile implants: semi-rigid and inflatable. Each works differently and has its own pros and cons.
A penile prosthesis is inserted through surgery. Before choosing your penile prosthesis, make sure you understand the surgery required, including the risks, complications and aftercare.
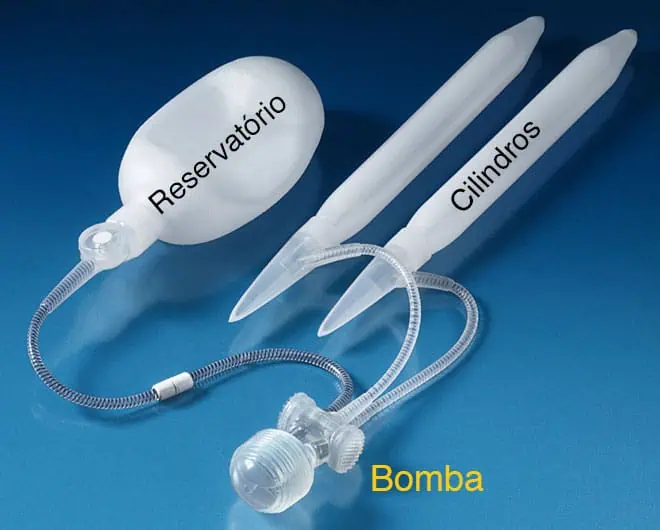
Inflatable Penile Prosthesis
The inflatable penile prosthesis is a surgical device that enables an impotent man to have an erection by transferring fluid from one part of the implant to another. The inflatable prosthesis is made up of three components: cylinders, a pump and a reservoir. All the components are implanted and generally cannot be seen outside the body.
The prosthesis cylinders are located on each side of the penis. They are inserted without the need to remove tissue. When they are filled with fluid, they expand and fill the penis, generating a physiological erection. The cylinders do not alter the sensitivity of the penis and allow the patient to continue to ejaculate. The head of the penis also continues to fill with blood (in cases where this was already the case before surgery). The liquid needed to fill the cylinders and generate an erection is stored in the reservoir, which is implanted inside the patient's stomach. The liquid is transferred by activating the pump, which is located in the scrotum.
The penile prosthesis provides the patient with an erection for as long as desired, and it is not interrupted by orgasm. When the patient wishes, the prosthesis can be deflated by pressing a “button” located on the top of the pump, along with compression of the penis. This action causes the fluid to return to the reservoir.
The prosthesis implantation can be performed through a single incision in the scrotal sac. Return to sexual activity typically occurs around 6 weeks post-surgery.
Semi-Rigid (Malleable) Penile Prosthesis
The semi-rigid penile prosthesis is a surgically implanted device that enables a man with erectile dysfunction to achieve an erection. It consists of two cylinders that are constantly firm but flexible, meaning they can be bent. All components are implanted and are generally not visible outside the body.
These cylinders occupy the space that was previously filled with blood during an erection. They do not affect penile sensitivity and allow the patient to continue ejaculating. The glans also continues to fill with blood (in cases where this occurred before the surgery).
When desired by the patient, the penis with the prosthesis can be “bent” to the side or another direction to make it less noticeable. The advantage of this prosthesis is that it does not require a pump or fluid reservoir to function, making it easier to use. The chance of mechanical failure is also lower. The disadvantage is that the “erection” is less physiological and continuous, although the penis can be bent.
Its placement is performed through an incision in the scrotal sac. Once the wound heals, it becomes barely noticeable.

Premature Ejaculation
We can consider premature ejaculation when the patient ejaculates very quickly after vaginal penetration or even before it occurs. The time considered is less than 1-2 minutes.
Premature ejaculation can be a lifelong condition or it can have started recently.
Many patients think they have premature ejaculation, but in fact they just lack knowledge of the normal time that elapses from the moment of penetration to ejaculation (TLEI - intravaginal ejaculatory latency time), which in normal men is 3-6 minutes.
It's interesting to note that there is a reduction in TLEI time as men get older. One study found that men aged 18-30 had an average TLEI time of 6.5 minutes, while men aged 51 had an average TLEI time of 4.3 minutes. Circumcision or the use of condoms do not alter this time.
The incidence of the disease is 22.5% of the male population. Affected men tend to have a higher sexual frequency than those without the disorder.
Vasectomy Without Cuts
Vasectomy is the fourth most used form of contraception in the United States, after condoms, the female pill and tubal ligation. When compared to the latter, vasectomy is just as effective, but simpler, faster, safer and cheaper. It takes less time off work and is performed under local anesthesia. Post-operative complications are less serious and rarer than those of tubal ligation1.
Currently, the recommended technique (used by Dr. Alexandre Miranda) is the non-scalpel vasectomy, as it has the following characteristics less chance of bleeding, pain during surgery, scrotal pain, infection and bruisingcompared to the traditional technique (with two small cuts). It also provides a faster recovery for returning to daily and sexual activities2.
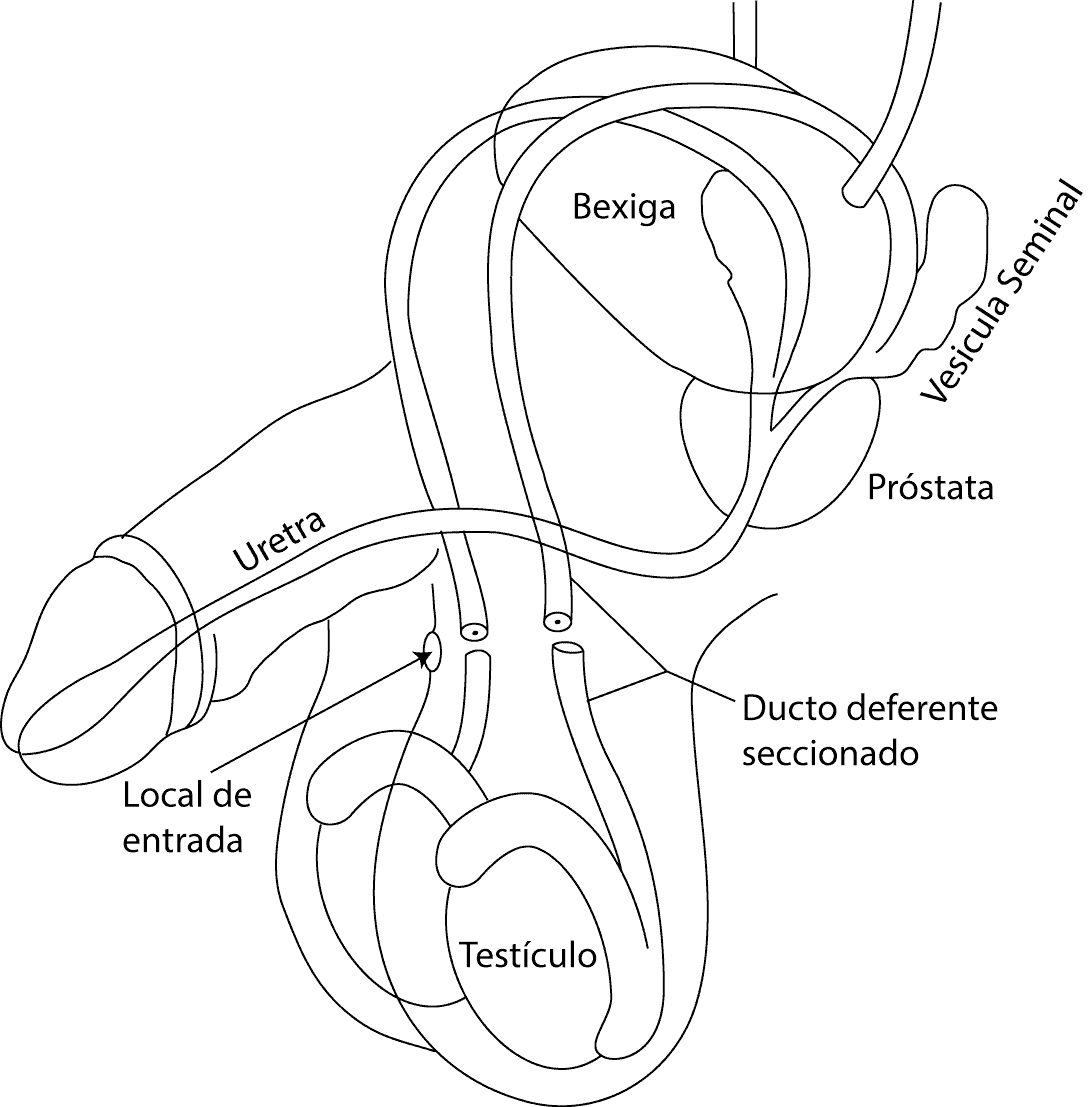
In the technique used by Dr. Alexandre Miranda the vas deferens (the tubes that connect the testicles to the urethra and through which the sperm pass) are accessed through the scrotum in one place, without any cuts. No stitches are required at the end of the procedure.
- Sharlip ID, Belker AM, Honig S, et al. Vasectomy: AUA guideline. The Journal of urology. 2012;188:2482-2491.
- Cook LA, Pun A, Gallo MF, Lopez LM, Van Vliet HA. Scalpel versus no-scalpel incision for vasectomy. The Cochrane database of systematic reviews. 2014;3:CD004112.
Advantages
Less pain
10x fewer complications
No points required
Faster recovery
Safe and effective birth control
Vasectomy is one of the safest and most effective definitive methods of birth control. It is safer and more effective than ligation performed by women.
The no-cut vasectomy technique is different from the traditional one: it doesn't require the use of a scalpel. The surgeon uses specific instruments to make a small hole through which the vas deferens (the tubes through which sperm pass) are cut, ligated and cauterized. The hole is so small that no stitches are needed to close it.
Questions and answers
Can I stop other contraceptive methods after the vasectomy?
No! Sperm can remain alive in the vas deferens, just above where it was cut and attached.
How will the vasectomy affect me?
Vasectomy is not castration. It just stops the flow of the tube that carries the sperm from the testicles to where it is mixed with your semen. Your penis and testicles will not be affected. All sexual and hormonal functions will continue unchanged, as will your voice, body hair and sexual interest. Studies show that patients who have had a vasectomy have more sex than those who haven't (1).
- Cook LA, Pun A, Gallo MF, Lopez LM, Van Vliet HA. Scalpel versus no-scalpel incision for vasectomy. The Cochrane database of systematic reviews. 2014;3:CD004112.
Is vasectomy a painful procedure?
No. You may feel some discomfort the moment the anesthetic is applied. Once it has taken effect, no pain is felt. During the procedure, some men may feel slight "tugging" due to the manipulation of the vas deferens. After the procedure you may be a little sore for a few days. Usually 2 to 3 days is the rest time needed to return to normal activities; only sexual activity should be resumed after 7 days.
Does vasectomy have any long-term risks?
Several studies have analyzed the long-term risks of vasectomy and none of them have shown any risks. Men who underwent vasectomy were NOT more likely to develop cancer, heart disease, sexual dysfunction (impotence) or any other health problems.
Can vasectomy be reversed?
In many cases, yes. However, it is a microsurgery with a result that is not guaranteed. Vasectomy should therefore be considered an irreversible sterilization procedure. If you're thinking of having it reversed now, it may not be the right time. Think about it a little more.
Vasectomy Reversal
It is estimated that 2-6% of men who have had a vasectomy want to have it reversed.
The surgery is carried out using a microscope and microsurgical material, as it is a microscopic procedure where the threads are thinner than a strand of hair.
The chance of pregnancy in patients who undergo reversal less than 3 years ago is 97%; between 3-8 years is 53%; between 9-14 years is 44% and over 15 years is 31%.
Dr. Alexandre Miranda has experience in vasectomy reversals. He is currently the head of the Andrology section at the Federal Hospital of Ipanema and responsible for reversals at the hospital.



